LiveTV is a free website where you can watch sports and games from all over the world as they happen. LiveTV lets you watch sports and games from all...
25 Best LiveTV Alternatives Free Sports Streaming Sites
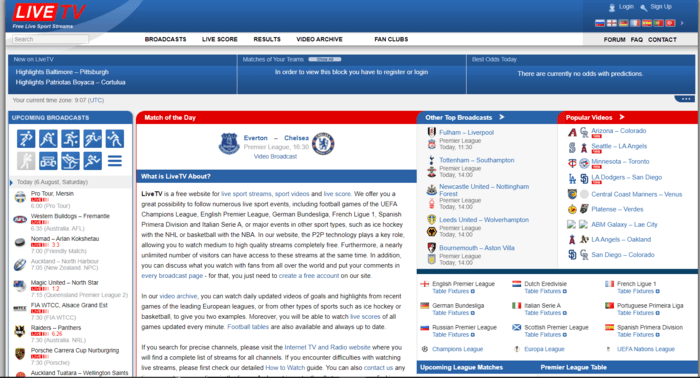
LiveTV is a free website where you can watch sports and games from all over the world as they happen. LiveTV lets you watch sports and games from all...


Microsoft will begin offering Windows 10 Update v1903 shortly now, and I am confident that the majority of you have to be excited about installing it as soon as...
This post will explain Benefits of social media for business. Remember when individuals stated social media was simply a trend? Its power has become...
Best and most authentic reason to call a Locksmith Services will be described in this article. Being locked out of your house or place of business can be very...
Welcome to AniWave, the ultimate portal for anime lovers. If you’re a fan of anime series and movies, you’ve come to the right place. AniWave...
Striven ERP is a resource planning software that assists firms in bringing their distant workers together and streamlining operations. Employees may work...
OMGChat comes to a free webcam support chatting platform called OMGcams. OMGChat is a free chatting community that allows people to interact with each other...
Nowadays watching sports is a popular leisure and it is consumed worldwide in various forms. It is an age-old practice now available via various means of...
Hurawatch is the go-to platform for streaming movies and series, providing users with an unparalleled entertainment experience. With its user-friendly...
Learn how to easily access and manage your Milestone credit card online by following these step-by-step instructions. Logging into your Milestone credit card...
Kisskh, the ultimate destination for all your Asian dramas and movies! If you’re a fan of captivating storytelling, gripping plots, and diverse cultural...